Research
Hormone Replacement Therapy in Adolescents with Premature Ovarian Insufficiency
POI is a rare condition, characterized by absent or irregular menstrual cycles, which represents a significant cause of infertility in women with estrogen deficiency before the age of 40. The etiology of POI includes chromosomal (Turner Syndrome, Fragile-X Syndrome), iatrogenic (chemotherapy, radiation, or surgery), autoimmune, or idiopathic (unknown) causes. POI has a complex clinical presentation with various health complications such as vasomotor or menopausal symptoms, infertility, decreased bone mineral density (BMD) leading to osteoporosis and increased fracture risk, as well as increased risk for cardiovascular, autoimmune diseases and mood disorders. Hormone Replacement Therapy (HRT), which is the physiologic replacement of premenopausal levels of estrogen and progesterone, is the most common treatment option for women with POI, that showed a positive effect on bone and cardiovascular health. However, there is a lack of controlled clinical trials in younger women with POI. Therefore, we are conducting the interventional study on adolescents with POI and characterize the most effective dosage, regimen, and choice of preparation of HRT for the treatment of this group of patients (ClinicalTrials.gov). We will thoroughly investigate the effects of therapy on multiple health outcomes. One of the aspects of this study is to investigate the skeletal phenotype examined using high-resolution peripheral quantitative computed tomography (HRpQCT), which is a cutting-edge imaging research tool that will provide valuable data on the bone microarchitecture and structure in adolescents with POI and will also allow us to follow changes of bones as a response to HRT. NIH has recently acquired an HRpQCT scanner, one of 28 scanners in North America.
High-resolution peripheral computed tomography
High-resolution Peripheral Quantitative Computed Tomography (HRpQCT) is a non-invasive, low-dose 3D imaging method used to evaluate volumetric bone mineral density and bone microarchitecture of peripheral skeletal sites, including distal radius and distal tibia. HRpQCT has an ability to differentiate between cortical and trabecular bone compartments providing density and structure parameters. It is a research tool that was found to improve prediction of fracture risk in the studies of primary and secondary osteoporosis, as well as endocrine disorders affecting bone and rare bone diseases. Our lab is one of the relatively small number of centers that has an HRpQCT scanner. Low dose, non-invasiveness and high resolution make HRpQCT a valuable tool in bone research. In several chronic disease models, we are examining the relationship between failure load and other HRpQCT–derived outcomes and fracture risk.
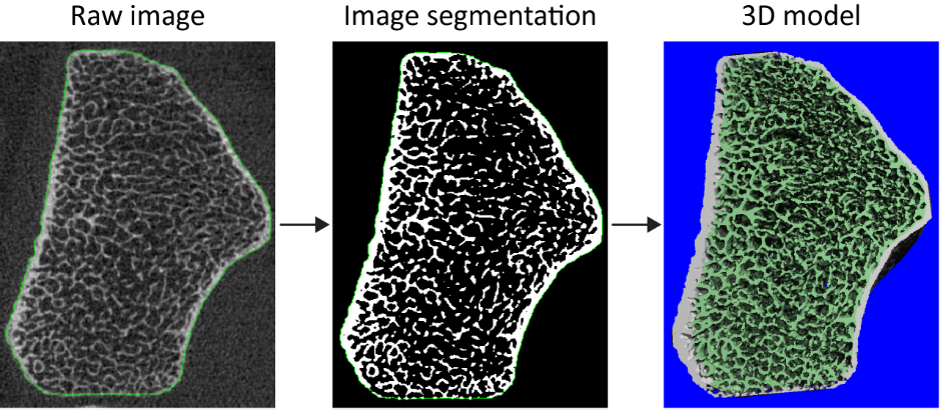
Evaluations of bone marrow composition
Our team is using magnetic resonance (MR) imaging and spectroscopy to evaluate bone marrow fat, an outcome that is directly influenced by hormonal signals. We have studied bone marrow composition in adolescents with anorexia nervosa and are employing this technique to examine the correlation between marrow fat and bone accrual in adolescents with inflammatory bowel disease and other pediatric clinical models. T1 maps and MR spectroscopy evaluations afford non-invasive means to evaluate bone marrow composition in children and adolescents.
 BACK TO TOP
BACK TO TOP