NIH scientists have shown that a common gene variant influences memory for events in humans by altering a growth factor in the brain's memory hub. On average, people with a particular version of the gene that codes for brain derived neurotrophic factor (BDNF) performed worse on tests of episodic memory - tasks like recalling what happened yesterday. They also showed differences in activation of the hippocampus, a brain area known to mediate memory, and signs of decreased neuronal health and interconnections. These effects are likely traceable to limited movement and secretion of BDNF within cells, according to the study, which reveals how a gene affects the normal range of human memory, and confirms that BDNF affects human hippocampal function much as it does animals'.
Michael Egan, M.D., Daniel Weinberger, M.D., National Institute of Mental Health (NIMH), Bai Lu, Ph.D., National Institute of Child Health and Human Development (NICHD) and colleagues, report on their discovery in the January 24 issue of Cell.
Long known to be critical for the growth and survival of neurons, BDNF has also recently been shown to play a key role in memory and hippocampal function in animals. To find out if it works similarly in humans, the researchers explored the consequences of a tiny variance in the human BDNF gene, where its molecular makeup differs slightly across individuals. People inherit two copies of the BDNF gene -- one from each parent - in either of two versions. Slightly more than a third inherit at least one copy of a version nicknamed "met," which the researchers have now linked to poorer memory. It's called "met" because its chemical sequence contains the amino acid methionine in a location where the more common version, "val," contains valine.
"We are finding that this one amino acid substitution exerts a substantial influence on human memory, presumably because of its effects on the biology of the hippocampus," said Weinberger.
Despite its negative effect on memory, the "met" version's survival in the human genome suggests that it "may confer some compensatory advantage in other biological processes," note the researchers. Although they found that it does not confer increased susceptibility to schizophrenia, they suggest that the "met" variant might contribute to risk for - or increase functional impairment in -- other disorders involving hippocampal dysfunction, such as Alzheimer's disease or mood disorders.
Drawing on participants in the NIMH intramural sibling study of schizophrenia, Egan and colleagues first assessed their hippocampal function and related it to their BDNF gene types.
Among 641 normal controls, schizophrenia patients, and their unaffected siblings, those who had inherited two copies of the met variant scored significantly lower than their matched peers on tests of verbal episodic (event) memory. Most notably, normal controls with two copies of "met" scored 40 percent on delayed recall, compared to 70 percent for those with two copies of "val." BDNF gene type had no significant effect on tests of other types of memory, such as semantic or working memory.
The researchers then measured brain activity in two separate groups of healthy subjects while they were performing a working memory task that normally turns off hippocampus activity. Functional magnetic resonance imaging (fMRI) scans revealed that those with one copy of "met" showed a pattern of activation along the sides of the hippocampus, in contrast to lack of activation among those with two copies of "val."
Next, an MRI scanner was used to measure levels of a marker inside neurons indicating the cell's health and abundance of synapses -- tiny junctions through which neurons communicate with each other. Again, subjects with one copy of "met" had lower levels of the marker, N-acetyl-aspartate (NAA), than matched individuals with two copies of "val." Analysis showed that NAA levels dropped as the number of inherited "met" variants increased, suggesting a possible "dose effect."
Unlike other growth factors, hippocampal BDNF is secreted, in part, in response to neuronal activity, making it a likely candidate for a key role in synaptic plasticity, learning and memory. To explore possible mechanisms underlying the observed "met"- related memory impairment, the researchers examined the distribution, processing and secretion of the BDNF proteins expressed by the two different gene variants within hippocampal cells. When they tagged the gene variants with green fluorescent protein and introduced them into cultured neurons, they discovered that "val" BDNF spreads throughout the cell and into the branch-like dendrites that form synapses, while "met" BDNF mostly clumps inside the cell body without being transported to the synapses. To regulate memory function, BDNF must be secreted near the synapses.
"We were surprised to see that 'met' BDNF secretion can't be properly regulated by neural activity," said Lu.
The observed memory decrements are likely traceable to the failure of "met" BDNF to reach the synapses, as well as its inability to secrete in response to neuronal activity, say the researchers.
"Our study provides direct in vivo data that the molecular mechanisms related to activity dependent BDNF secretion and signaling, such as synaptic plasticity, may underlie humans' greatly expanded verbally-mediated memory system, just as it does for more rudimentary forms of memory in animals," said Egan.
In following-up their leads, the researchers are searching for a possible BDNF connection with the memory problems and hippocampal changes of Alzheimer's disease, depression and normal aging.
Also participating in the study were: Drs. Joseph Callicott, Terry Goldberg, Bhaskar Kolachana, Alessandro Bertolino, NIMH; Drs. Masami Kojima, Eugene Zaitsev, NICHD; Dr. David Goldman, National Institute on Alcohol Abuse and Alcoholism (NIAAA); Drs. Bert Gold, Michael Dean, National Cancer Institute (NCI).
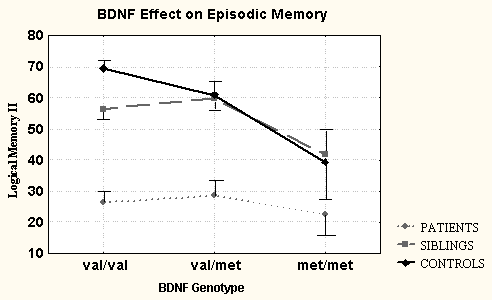
Graph shows the effect of BDNF gene type on performance during a test of delayed recall of memory for events among 641 participants in the NIMH Clinical Brain Disorders Branch sibling study of schizophrenia. Normal controls (heavy black line) who had inherited two copies of "met" scored 40 percent, compared to 70 percent for those with two copies of "val."
Source: NIMH Clinical Brain Disorders Branch
###
NIMH, NICHD, NIAAA and NCI are part of the National Institutes of Health (NIH), the Federal Government's primary agency for biomedical and behavioral research. NIH is a component of the U.S. Department of Health and Human Services.
 BACK TO TOP
BACK TO TOP