The pores created by malaria parasites to exit red blood cells are promising targets for drugs such as heparin, according to a new study led by researchers at NIH’s Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD). The results offer a new approach for targeting malaria parasites, including drug-resistant strains. The findings appeared in the September 25, 2017, online issue of Scientific Reports.
Background
Malaria is a serious, flu-like illness caused by parasites that spread to people from the bite of an infected mosquito. According to the World Health Organization, there were 212 million new cases of malaria worldwide in 2015, with an estimated 429,000 malaria deaths. Young children under 5 years of age are particularly vulnerable to severe outcomes such as anemia, liver problems, and seizures and accounted for approximately 303,000 deaths globally.
Currently, artemisinin and related drugs are effective malaria treatments, but in five countries, the parasite has developed resistance to them. In the 1950s, malaria parasites became resistant to chloroquine, rendering the treatment virtually useless. Because resistance presents an ongoing problem, new therapies are needed, especially treatments that target most or all disease-causing species and strains of the parasite. Of these, Plasmodium falciparum causes the most malaria deaths.
Results
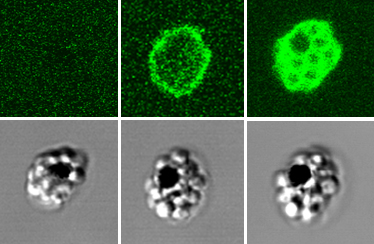
Researchers led by NICHD’s Joshua Zimmerberg, M.D., Ph.D., explored the anti-malaria properties of heparin, a drug typically used to prevent or treat blood clots that has shown the ability to impair malaria parasites in laboratory experiments. Using time-lapse microscopy and other techniques, the team discovered that heparin blocked the ability of P. falciparum to leave red blood cells, where parasites multiply before exiting to infect new cells.
The researchers found that heparin worked at a specific step—after the parasites formed pores in red blood cells but before the cells burst open. The team showed that heparin prevented parasites from separating from each other, likely by binding to a parasite protein called MSP1 and kept the cell’s membrane from rupturing. Importantly, they also found that heparin worked against artemisinin-resistant strains of parasites.
Significance
“By entering through the short-lived pores, heparin exploits a previously unrecognized vulnerability in the malaria parasite’s life cycle,” said Dr. Zimmerberg. “Researchers could target this step by developing new drugs optimized for this purpose.”
Overall, a better understanding of how malaria parasites exit and disperse from red blood cells may offer additional drug targets, especially against drug-resistant strains.
Reference
Glushakova S, Busse B, Garten M, Fairhurst RM, Goldberg DE, and Zimmerberg J. Exploitation of a newly-identified entry pathway into the malaria parasite-infected erythrocyte to inhibit parasite egress. Scientific Reports DOI: 10.1038/s41598-017-12258-x (2017)
 BACK TO TOP
BACK TO TOP